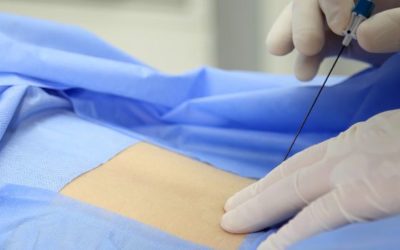
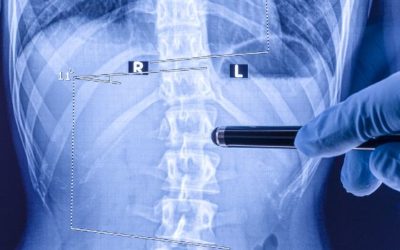
Did you know that Advanced Pain Medical Group offers celiac plexus block treatments at our eight Southern and Central California locations? Some conditions can cause intense abdominal aches and can become unbearable. Fortunately, a celiac plexus block can sometimes...
Treatments
Diagnostic Medial Branch Block
If you have back or neck pain or irritated joints, your doctor may recommend several tests to find the source of the problem. These tests may include a diagnostic medial branch block. To make the most informed decisions for your health, it's important to understand...
Facet Joint Injections
Advanced Pain Medical Group provides facet joint injections at eight locations in Los Angeles, Kern, and Ventura counties. If facet joint inflammation is behind your chronic back pain, sore neck, or headaches, we may be able to help. Read on to learn what this...
Lumbar Sympathetic Nerve Block
If you’re struggling with debilitating lower back or leg pain and regular pain meds aren’t cutting it, a lumbar sympathetic nerve block at Advanced Pain Medical Group in California may help. This minimally invasive procedure targets the pain at its source, doesn’t...
PRP Injections For Pain
Platelet-rich plasma therapy, also known as PRP therapy, brings relief to many people worldwide. This non-surgical technique is highly effective for many conditions and can be a successful alternative to opioid prescriptions. What is Platelet-Rich Plasma Therapy?...
Radiofrequency Ablation
If you are researching pain management options in the Los Angeles area, you may want to consider radiofrequency ablation. This noninvasive treatment applies radio waves to damaged nerves, blocking them from sending pain signals to your brain. You may find relief with...
Radiofrequency Neurotomy
If you've been experiencing chronic pain that won't respond to standard treatment, Advanced Pain Medical Group offers radiofrequency ablation for patients in Kern, Los Angeles, and Ventura County. Radiofrequency neurotomy (or “rhizotomy”) is a minimally invasive...
Sacroiliac Joint Steroid Injection
Anyone with problems with their sacroiliac joint may need to treat the inflammation to move comfortably again. Advanced Pain Medical Group in the Los Angeles, Kern, or Ventura County areas can help patients who need help improving their quality of life. What Is The...
Spinal Cord Stimulation
When other pain management methods fail, spinal cord stimulation (SCS) offers a non-surgical, drug-free solution for chronic back pain. Advanced Pain Medical Group's pain clinics in the Los Angeles, CA metro area offer this specialized treatment. SCS prevents the...
Stellate Ganglion Block For Pain
If you are looking for a fast-acting neck pain treatment, consider getting a stellate ganglion block at an Advanced Pain Medical Group clinic in California. Our specialists have years of training and clinical experience diagnosing and treating complex forms of pain...
Stem Cell Therapy For Pain
At Advanced Pain Medical Group in Los Angeles, Kern, and Ventura Counties, our specialists have many years of experience diagnosing the complex causes of pain. We are at the forefront of administering cutting-edge treatments, including stem cell therapy, to help our...
Nerve Blocks & Epidural Treatment
Living with chronic pain can significantly impact daily life, hindering mobility, and diminishing overall wellbeing. Fortunately, modern medicine offers effective solutions for managing pain, including nerve blocks and epidurals. Learn more about these procedures and...
Steroid Injections
Many residents of Southern California choose to receive back pain treatment at Advanced Pain Medical Group to manage their chronic pain, chiropractic conditions, and general discomfort. One of the most common procedures at the Pain Clinic is steroid injections. What...
Lumbar Transforaminal Epidural Steroid Injection
Advanced Pain Medical Group treats adults in Los Angeles, Kern, and Ventura County experiencing back pain with a potent solution — Lumbar Transforaminal Epidural Steroid Injection (LTESI). Understanding Lumbar Transforaminal Epidural Steroid Injection LTESI is a...
Cervical Epidural Steroid Injections
Advanced Pain Medical Group offers cervical epidural steroid injections (CESI) at our eight locations in Los Angeles, Kern, and Ventura counties. Neck pain can be debilitating and interfere with daily activities. CESI is a minimally invasive neck pain treatment option...
Caudal Epidural Steroid Injection
Caudal Epidural Steroid Injections are one option for pain management at Advanced Pain Medical Group in Los Angeles, CA. This safe and effective treatment is tailored for adults dealing with significant lower back or leg pain, commonly associated with conditions such...
Vertiflex Superion Spinal Decompression
If you're currently suffering from lumbar spinal stenosis and need help to recover, a pain management specialist at Advanced Pain Medical Group in Los Angeles can help. Through new treatments including Vertiflex Superion Spinal Decompression, you can feel long-lasting...
Lumbar Discography
Advanced Pain Medical Group is a premier provider of pain management solutions for adults experiencing lumbar pain in Los Angeles, Kern, and Ventura Counties. One of our leading diagnostic services is Lumbar Discography – an invaluable diagnostic test that aids in...